| 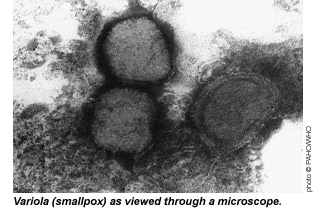 Smallpox is a very serious, contagious and sometimes fatal
disease caused by a virus (variola); it characteristically includes skin
lesions and scabs that, at times, have been confused for chickenpox. The
disease occurs only among humans and is passed from person to person. Smallpox
can cause a severe rash over the whole body that can leave scars. Other
symptoms include high fever and severe headache or body aches. Death occurs in
about 30 percent of infected people. Some survivors may suffer blindness. Smallpox is a very serious, contagious and sometimes fatal
disease caused by a virus (variola); it characteristically includes skin
lesions and scabs that, at times, have been confused for chickenpox. The
disease occurs only among humans and is passed from person to person. Smallpox
can cause a severe rash over the whole body that can leave scars. Other
symptoms include high fever and severe headache or body aches. Death occurs in
about 30 percent of infected people. Some survivors may suffer blindness.
How common is
smallpox?
The disease was declared eradicated from the Earth in
1980 following a worldwide vaccination program. The last naturally acquired
case of smallpox in the world occurred in 1977 in Somalia. The last case in the
United States was in 1949 and the last cases in Illinois were recorded in 1947.
All known variola virus stocks are held frozen in secure facilities at the U.S.
Centers for Disease Control and Prevention (CDC) and at a state research center
in Russia.
Why should I be concerned about
smallpox?
At this time, there is no evidence of an imminent threat
that terrorists might use smallpox as a biological weapon. However, the events
of September and October 2001 heightened awareness of the possibility of
deliberate terrorist attacks that could include smallpox or other biological
agents. Because of the potential that secret stockpiles of smallpox might exist
in other countries and could fall into the hands of terrorists, it is important
that the American people are protected against the threat of a smallpox attack
and that health care workers and others are familiar with the clinical features
of the disease. While the possibility of an intentional release of smallpox
virus is low, the consequences of an outbreak would be great.
Is there a vaccine for
smallpox?
Yes. The vaccine is made from a live virus related to
smallpox that helps the body develop immunity to smallpox. The vaccine does not
contain smallpox virus and cannot spread the disease. The government reserve of
vaccine, which was produced in the 1970s, is sufficient to inoculate every
American in the event of a smallpox attack. Production of a new smallpox
vaccine is underway and is expected to be available by 2004. Routine
vaccinations in the U.S. were discontinued in 1972 because it was no longer
necessary for prevention.
Are smallpox
vaccinations going to resume?
President George W. Bush recently unveiled a plan to
immediately begin to vaccinate 500,000 military personnel who may be deployed
in high threat areas. In addition, beginning in 2003, the vaccine will be
offered to as many as 10 million civilian public health and hospital workers,
including 10,000 in Illinois, who will make up special smallpox response teams.
A second phase, starting in the spring of 2003, includes offering the vaccine
to all hospital workers not included in the first phase and to first responders
(firefighters, police officers and emergency medical service personnel). A
third phase, beginning sometime in 2003, would make the vaccine available to
the general public.
What will the public health
response teams do?
These individuals would investigate and evaluate
suspected cases of smallpox and initiate measures to control an outbreak.
Public health personnel at the state, regional and local levels would
investigate/control a possible or actual smallpox case or outbreak, or would be
available to vaccinate others. The hospital workers who form health care teams
would diagnose and treat possible or actual cases of smallpox. Participation on
these teams and in the vaccination program is voluntary.
Why can't the public get the
vaccine?
While it has been strongly recommended that the public
not seek the vaccination now, because there is no imminent danger of a smallpox
attack, President Bush has said plans are being formulated to accommodate those
adult members of the public who insist on being vaccinated.
How safe is the smallpox
vaccine?
The smallpox vaccine is the best protection you can get
if you are exposed to the smallpox virus. However, without evidence of an
actual case of smallpox, the vaccine is not recommended because it does have
serious side effects. Based on data from 1968 when the vaccine was widely
given, federal health authorities have predicted that, for every million people
vaccinated, one or two people may die from the vaccination, 14 to 52 would
experience life-threatening reactions and about 1,000 would develop serious,
but not life-threatening, reactions. In addition, the vaccine requires a series
of pricks that create an open sore and, until the sore forms a scab, the
vaccinia virus can spread and cause infection in the person who received the
vaccine or in family members and other close contacts.
Are there other less serious
side effects to the vaccine?
Yes. Up to 20 percent experience headache, fatigue,
muscle aches, pain or chills after smallpox vaccination, usually about eight to
12 days later. Some individuals may have rashes that last two to four days.
These side effects are usually temporary and go away on their own or with
minimal medical treatment, such as aspirin and rest.
Are there people who should NOT
get the vaccination?
Some people are at greater risk for serious side effects
from the smallpox vaccine and those who have any of the following conditions,
or live with someone who does, should NOT receive the smallpox vaccine unless
they have been exposed to the smallpox virus.
- Eczema or atopic dermatitis (This is true even if the
condition is mild or not currently active, or if it was experienced as a
child.)
- Skin conditions such as burns, chickenpox, shingles,
impetigo, herpes, severe acne or psoriasis (People with any of these conditions
should not get the vaccine until they have completely healed.)
- Weakened immune system (Cancer treatment, an organ
transplant, HIV/AIDS or medications, such as steroids, to treat autoimmune
disorders and other illnesses can weaken the immune system.)
- Pregnancy or plans to become pregnant within one month
of vaccination
In addition, individuals should not get the smallpox
vaccine if they are allergic to the vaccine or any of its ingredients, are
younger than 12 months of age, have a moderate or severe short-term illness
(these people should wait until they are completely recovered) or are currently
breastfeeding.
As a precautionary step, if you have been diagnosed by a
doctor as having a heart condition with or without symptoms you should NOT get
the smallpox vaccine at this time while experts continue their investigations.
These include conditions such as:
- known coronary disease including:
- previous myocardial infarction (heart attack)
- angina (chest pain caused by lack of blood flow to the
heart)
- congestive heart failure
- cardiomyopathy (heart muscle becomes inflamed and
doesn't work as well as it should)
- stroke or transient ischemic attack (a
"mini-stroke" that produces stroke-like symptoms but no lasting
damage)
- chest pain or shortness of breath with activity (such as
walking up stairs)
- other heart conditions under the care of a doctor
In addition, you should NOT get the smallpox vaccine if
you have 3 or more of the following risk factors:
- You have been told by a doctor that you have high blood
pressure.
- You have been told by a doctor that you have high blood
cholesterol.
- You have been told by a doctor that you have diabetes or
high blood sugar.
- You have a first degree relative (for example mother,
father, brother, or sister) who had a heart condition before the age of 50.
- You smoke cigarettes now.
These may be temporary exclusions and may change as more
information is gathered.
The presence of these conditions in a close contact (such
as people you live with) is not a reason for you to defer vaccination.
Every person volunteering to receive the smallpox vaccine
will be asked detailed questions regarding his/her medical history and physical
health.
How is the vaccine
given?
The smallpox vaccine is not given with a hypodermic
needle and is not a "shot" like many vaccinations given today. The
vaccine is delivered using a bifurcated (two-pronged) needle that is dipped
into the vaccine solution. When removed, the needle retains a droplet of the
vaccine. The needle is then used to quickly prick the skin about 15 times in a
few seconds. The pricking is not deep, but it will cause a sore spot and one or
two drops of blood to form. The vaccine is usually given in the upper arm, but
can be given in the upper thigh.
If successful, a red and itchy bump develops at the
vaccination site in three or four days. In the first week after vaccination,
the bump becomes a large blister, fills with pus and begins to drain. During
week two, the blister begins to dry up and a scab forms. The scab falls off in
the third week, leaving a small scar. People who are being vaccinated for the
first time may have a stronger successful reaction than those who are being
revaccinated.
Are people who were vaccinated
in the past protected against smallpox?
The level of immunity, if any, among persons who were
vaccinated before 1972, when routine vaccination against smallpox ended, is
uncertain. About half of the U.S. population has been vaccinated and may have
partial immunity at best. Immunity can be boosted effectively with a single
revaccination. Prior infection with the disease results in lifelong immunity.
How long does a smallpox
vaccination last?
Past experience indicates the first dose of the vaccine
offers protection from smallpox for three to five years, with decreasing
immunity thereafter. If a person is vaccinated again later, immunity lasts
longer.
Is it possible to get smallpox
from the vaccination?
No, smallpox vaccine does not contain the smallpox
virus. Another related live virus, called vaccinia virus, is used in the
vaccine to provide immunity.
Can you get vaccinia from the
vaccination?
Because the vaccinia virus is live, it can spread to
other parts of the body or to other people from the vaccine site. It is spread
by touching the vaccination site before it has healed or by touching bandages
or clothing that have become contaminated with live virus from the vaccination
site. Vaccinia is not spread through the air. To prevent the spread of
vaccinia, don't touch the vaccination site or materials that touched it. If you
do touch the site or materials that have been in contact with the site, wash
your hands right away. Don't let others touch your vaccination site or
materials that have touched it.
What are the symptoms of
vaccinia?
Symptoms may include rash, fever, and head and body
aches.
If you are exposed to smallpox,
is it too late to get a vaccination?
Vaccination within three days of exposure will
completely prevent or significantly modify smallpox in the vast majority of
persons. Vaccination four to seven days after exposure likely offers some
protection from the disease or may moderate the disease's severity.
If someone receives the vaccine
now, will they need to be revaccinated if there is an attack?
In a post-attack emergency, to ensure everyone is
protected as rapidly as possible, all exposed persons will be vaccinated
regardless of smallpox vaccine history.
Who would get smallpox vaccine
in the event of an actual smallpox attack?
Anyone directly exposed to the smallpox virus should get
the vaccine, regardless of their health status, because a negative reaction to
the vaccine would be less severe than developing smallpox. Illinois public
health officials, working with federal health authorities, have developed a
plan to vaccinate everyone in the state in the event of smallpox outbreak.
There is enough smallpox vaccine to vaccinate everyone who would need it in the
event of an emergency.
How is smallpox
transmitted?
In most cases, smallpox is spread by an ill person to
others through infectious saliva droplets. Generally, direct and fairly
prolonged face-to-face contact is required to spread smallpox from one person
to another. People with smallpox are most infectious during the first week of
illness because that is when the largest amount of virus is present in saliva.
However, some risk of transmission lasts until the disappearance of all scabs.
Contaminated clothing or bed linen also could spread the virus. Special
precautions need to be taken to ensure all bedding and clothing of those
infected are cleaned appropriately with bleach and hot water. Disinfectants
such as bleach can be used for cleaning contaminated surfaces.
If used in biowarfare, smallpox virus could be dispersed
in the air and potential victims in the area of the release would breathe in
the virus, or infected persons could be sent into a crowded area to attempt to
spread the disease to others. If an aerosol release of smallpox occurs, 90
percent of the virus will be inactivated or dissipated in about 24 hours.
Smallpox is not known to be transmitted by insects or animals.
What are the symptoms of
smallpox?
Incubation period (duration 7-17 days; not
contagious) Following exposure to the virus, there is an incubation period of
about 12 days during which a person usually feels fine.
Initial symptoms (prodrome) (duration 2-4 days;
sometimes contagious) The first symptoms of smallpox to emerge are fever (101
degrees F to 104 degrees F), malaise, head and body aches and, sometimes,
vomiting.
Early rash (duration about 4 days; most
contagious) A rash begins to first emerge as small red spots on the tongue and
in the mouth. These spots develop into sores that break open and spread large
amounts of virus into the mouth and throat. The person becomes contagious at
this point.
As the sores in the mouth begin to break down, a rash
appears on the skin, starting on the face and spreading to the arms and legs
and then to the hands and feet. Usually the rash spreads to all parts of the
body within 24 hours. As the rash appears, the fever usually falls and the
person may start to feel better.
By the third day, the rash becomes raised bumps. By the
fourth day, the bumps fill with a thick, opaque fluid and often have a
depression in the center that resembles a bellybutton. (This is a major
distinguishing characteristic of smallpox.) Fever often will rise again at this
time and remain high until scabs form over the bumps.
Pustular rash (duration about 5 days; contagious)
The bumps become pustules – sharply raised, usually round and firm to the
touch as if there's a small round object (for example, a BB pellet) under the
skin.
Pustules and scabs (duration about 5 days;
contagious) The pustules begin to form a crust and then a scab. By the end of
the second week after the rash appears, most of the sores will have scabbed
over.
Resolving scabs (duration about 6 days;
contagious) The scabs begin to fall off, leaving marks on the skins that
eventually become pitted scars. Most scabs will have fallen off three weeks
after the rash appears. The person is contagious until all the scabs have
fallen off.
Scabs resolved (not contagious) Scabs have fallen
off and the person is no longer contagious.
If someone has a rash, how do
you determine if it is smallpox or chickenpox?
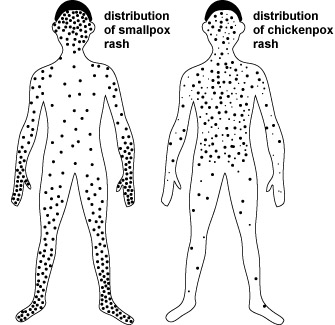 If someone
has a rash, how do you determine if it is smallpox or chickenpox? Smallpox can
be confused with chickenpox because of the presence of a rash. There are,
however, significant differences in the rash that accompanies each disease. The
chickenpox rash, which is usually not preceded by illness, is more prominent on
the trunk of the body and is almost never present on the palms of the hands or
the soles of the feet. Smallpox lesions, which are almost always preceded by
illness with a high fever, are more numerous on the face, arms and legs, and
the rash or pocks are usually present on the palms and soles. The chickenpox
rash consists of small groupings of fluid-filled blisters that appear and
progress to scabs at different rates over the course of the illness. It is not
unusual for a person with chickenpox to have both the blisters and the
resulting scabs present in the same area at the same time. The smallpox lesions
in a specific area, though, all appear to be at the same stage of development. If someone
has a rash, how do you determine if it is smallpox or chickenpox? Smallpox can
be confused with chickenpox because of the presence of a rash. There are,
however, significant differences in the rash that accompanies each disease. The
chickenpox rash, which is usually not preceded by illness, is more prominent on
the trunk of the body and is almost never present on the palms of the hands or
the soles of the feet. Smallpox lesions, which are almost always preceded by
illness with a high fever, are more numerous on the face, arms and legs, and
the rash or pocks are usually present on the palms and soles. The chickenpox
rash consists of small groupings of fluid-filled blisters that appear and
progress to scabs at different rates over the course of the illness. It is not
unusual for a person with chickenpox to have both the blisters and the
resulting scabs present in the same area at the same time. The smallpox lesions
in a specific area, though, all appear to be at the same stage of development.
Chickenpox is generally a mild illness characterized by a
slight fever, itchy bumps that turn into blisters and some generalized
discomfort. A patient with smallpox is very ill, has a high temperature and,
often, is unable to even rise from bed.
Is smallpox
fatal?
The majority of patients with smallpox recover, but
death may occur in up to 30 percent of cases.
Is there a treatment for
smallpox?
There is no proven treatment for smallpox, but research
to evaluate new antiviral agents is ongoing. Patients with smallpox can benefit
from supportive therapy (intravenous fluids, medicine to control fever or pain,
etc.) and antibiotics for any secondary bacterial infections that occur.
If someone comes down with
smallpox, how can the spread of the disease be stopped?
In the unlikely event that smallpox is reintroduced, the
public health system would be mobilized to trace all known contacts of the
infected person and vaccinate them to prevent more cases of smallpox from
developing. You can avoid getting the disease by avoiding contact with people
who have the disease. Because a person can spread smallpox from the time he or
she develops a rash until the rash has completely healed, these patients should
be placed in medical isolation so they will not continue to spread the virus.
In addition, people who have come into close contact with smallpox patients
should be vaccinated immediately and closely watched for symptoms of the
disease. Vaccination and isolation are the strategies to stop the spread of
smallpox.
If smallpox is discovered or
released in a building, how can that area be decontaminated?
The smallpox virus is fragile. In the event of an
aerosol release of smallpox, all virus will be inactivated or dissipated within
one to two days. Buildings exposed to the initial aerosol release of the virus
do not need to be decontaminated. By the time the first cases are identified,
typically two weeks after the release, the virus in the building will be gone.
Infected patients, however, will be capable of spreading the virus and possibly
contaminating surfaces while they are sick. Therefore, standard hospital-grade
disinfectants, which are effective in killing the virus on surfaces, should be
used for disinfecting hospitalized patients' rooms or other contaminated
surfaces.
What should people do if they
suspect someone with smallpox or suspect that smallpox has been released in
their area?
Report suspect cases of smallpox immediately to your
local health department or to the Illinois Department of Public Health. If you
believe there has been an intentional release of smallpox virus, also contact
your local law enforcement agency.
|

